March 1961 Lynwood, CA
When I was in the second grade my family bought a station wagon, a brand new Ford Falcon that seemed at the time like the most exciting thing that had ever happened to us. The bulbous old Plymouth now looked like a cartoon next to this spare, bronze bullet into the future.
The Falcon’s bench seats were upholstered in tawny vinyl, stamped in a western motif so that if you were wearing shorts, you’d leave the car with tiny white brands on the backs of your legs. The sheet-metal dashboard was painted metal-flake caramel, and it bristled with hard plastic knobs that you pulled and twisted to control everything from the choke to the windshield wipers. There were no seat belts and no headrests. On long drives, we kids wrestled and slept in the “way back,” with the dog and the ice chest.
The Falcon had all the safety features standard for its time. High-speed collisions in those days were horrific.
The Falcon was built just before a wave of major changes in automobile safety design. With more drivers on the road than ever before, and with funding boosted by the technology race with Communism, the 60s saw a surge of research on the mechanics of head injury, paid for by the car and airplane industries and by the federal government through branches including the National Institutes of Health (NIH), the National Air and Space Administration, and the Department of Defense. Out of this work grew seat belts, headrests, padded dashboards, and other innovations that reduced by three-quarters the nation’s transportation death rate per mile traveled between 1963 and 2003.[1]

From “Experimental Cerebral Concussion in the Rhesus Monkey,” Philip Yarnell & Ayub Ommaya, Bulletin of the New York Academy of Medicine, Vol. 45, No. 1, January 1969, p41
Primate research was very big at first. In a series designed to mimic rear-end collisions,[2] for example, monkeys were strapped into little carts and accelerated along a track by a sudden impact from behind. Recording the events with high-speed cameras allowed researchers to measure the whiplash effect on the animals’ unsupported necks. Among other things, these studies demonstrated that acceleration alone, without impact, could not only cause the loss of consciousness commonly known as concussion but also leave physiological trauma markers like subdural hematoma and cerebral edema (bleeding and swelling inside the skull).
Key to brain injury, researchers demonstrated, was the magnitude of the angular acceleration, that is, the acceleration of the head through the arc of the circle defined by the pivot point in the subject’s neck. Fitting the monkeys with cervical collars enabled the subjects to endure more force—or the same force for a longer time—before concussion became inevitable.[3]

An earlier helmet-trauma device, from “Cerebral Concussion and Traumatic Unconsciousness,” Ayub K. Ommaya and T.A. Gennarelli, Brain, 1974; 97: 640
At the University of Pennsylvania head-injury lab, a team led by neurosurgeon Thomas Gennarelli and biomechanical engineer Lawrence Thibault subjected 45 primates to head acceleration without impact, by means of a helmet dubbed the “Penn II device,” to develop what they called a model of head injury that would “duplicate the entire spectrum of traumatic unconsciousness described in human beings.”[4] They manipulated the magnitude, duration, and direction of acceleration to create comas of varying length and depth, and they demonstrated that acceleration alone could produce direct damage to the neurons, which were presumably being stretched beyond the limits of their material properties. This kind of nerve damage, known as Diffuse Axonal Injury (DAI), represents permanent loss of brain function.
Axonal injury routinely results from the swelling and oxygen deprivation that typically accompany traumatic brain injury, but Gennarelli et al. produced it as a primary effect of acceleration alone. Their data also supported the prediction that animals with larger heads were more vulnerable than animals with smaller heads to the effects of angular acceleration.
The papers were appearing in prestigious medical journals, the results reported at academic and industry meetings.[5] Then the nature of the research changed forever, after a public and acrimonious struggle that tainted everybody involved.
First came the Silver Spring monkeys, a pathetic group of macaques used in a stroke-recovery experiment funded by the NIH. Scientists at the Institute for Behavioral Research in Silver Spring, Maryland, had severed the nerves to the animals’ forelimbs, to see whether their subjects could remap the surrounding brain cells and regain control of the numb and useless arms—if that was the only way they could reach food.
An animal-rights activist named Alex Pacheco had heard of the experiment and joined the lab staff as a volunteer. He began coming in alone at night, which is when he took many of the pictures he turned over to local police, who decided to raid the lab on animal cruelty charges. Tipped off by Pacheco, a television crew and a number of print reporters arrived at the raid shortly after the officers, and the resulting publicity vaulted the story to the national arena. Although the case was eventually tossed out by the Maryland Supreme Court, the publicity surrounding the raid and the initial conviction of the lab’s director fueled the exploding animal-rights movement and established Pacheco’s organization, People for the Ethical Treatment of Animals (PETA), as a major force.
For two years after the Silver Spring raid, while the Maryland scientists appeared to be losing in the criminal courts, Gennarelli et al. continued their work with primates at the University of Pennsylvania. This time the doctors were nailed with their own videotapes, stolen in a late-night break-in by the Animal Liberation Front and fed to the media by PETA. The tapes showed not only the violent and debilitating shaking of the captive animals, but also the attaching of the helmet and sensors beforehand, and the handling of the injured animals afterwards. Like Stanford students in the Zimbardo prison study[6] or soldier-guards at Abu Ghrayab, the researchers in the Penn head-injury labs were not as respectful of their captives’ dignity as most of us would like.
And so it was that, after an unpleasant and highly publicized sequence of legal actions, illegal actions, professional embarrassment, and political pressure, the head-injury lab at the University of Pennsylvania Department of Bioengineering lost federal funding, at least for the time being, and a number of brilliant scientists were available for another kind of research.
In 1984, the year the tapes were stolen from the Department of Bioengineering, Dr. Ann-Christine Duhaime was a neurosurgery resident at the University of Pennsylvania School of Medicine. Her faculty advisor was Dr. Derek Bruce, a neurosurgeon who’d been among the first to explore the use of Computer-Aided Tomography (CAT, or CT scans) in the context of brain injury. The technology was very exciting, Bruce recalled in a telephone interview in 2003, because doctors could finally see what was happening inside the head of an unconscious patient without opening up the skull. CT scans can look past the bones, at the soft tissue beneath, and especially at blood flow.
The doctors quickly noticed a certain category of very young patient with impaired consciousness and pools of subdural bleeding. Like generations of physicians before him, Bruce found himself alone with desperate parents on late-night vigils. “These people were not monsters,” Bruce says, “They clearly did care about their children.” When he heard about Caffey’s proposition that whiplash shaking could cause subdural hematoma, though, he began asking more questions, trying to draw out the parents about what might have happened. A surprising number of them confessed, he says, not to beating or battering, but to shaking the child, or maybe throwing the infant onto a soft surface, like a crib or sofa.
Derek Bruce had resigned himself to the apparent reality that even loving parents can under stress shake their children hard enough to cause serious and permanent brain damage, possibly without leaving any other signs of violence. His opinion was an irritation to one of his young residents, Tina Duhaime.
“She used to get mad at me. She felt I was being unfair to the parents,” Bruce remembers. “I would say, ‘It’s an inflicted injury,’ and she would say, ‘How do you know?’ She was going into her research year, and so I told her, ‘Put together a study. Let’s find out.’”
Which is how a young graduate student, Ann-Christine Duhaime, became the defining name on a landmark paper, “The Shaken Baby Syndrome: A Clinical, Pathological, and Biomechanical Study,” [7] which is still one of the most quoted documents in the field.
She and Dr. Bruce had pulled together a crack team: Engineer Lawrence Thibault was a veteran of not only the Penn primate labs but also the Navy’s work with crash-test dummies. He designed for Duhaime a set of dolls intended to model one-month-old infants, with wet-cotton brains, flexible spines, and implanted accelerometers. Volunteers took turns shaking the dolls, and Duhaime compared the measured forces with the thresholds for primate concussion established by Gennarelli et al., extrapolated to predict injury levels to human infants.
“What Tina found was that shaking by a normal adult didn’t cause nearly enough acceleration to produce these injuries,” Bruce says. “That’s when we added the impact series.”
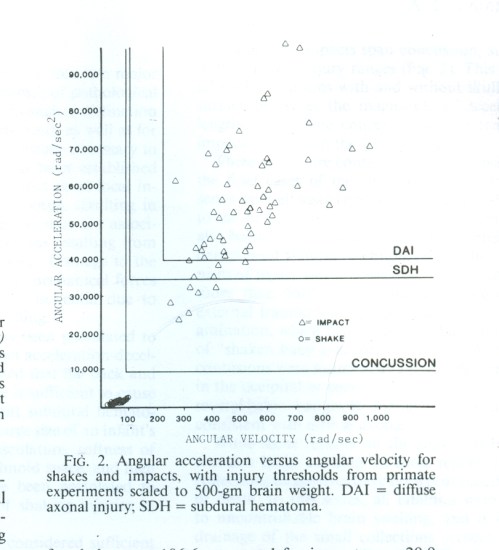
From “The shaken baby syndrome: A clinical, pathological, and biomechanical study,” Ann-Christine Duhaime, M.D., Thomas A. Gennarelli, M.D., Lawrence E. Thibault, Sc.D., Derek A. Bruce, M.D., Sudsan S. Margulies, M.S.E., and Randall Wiser, M.S.E., Journal of Neurosurgery, Vol. 66, March 1987, p. 413. The cluster of dots in the lower-left corner is the shaking data.
Again, volunteers shook the dolls as hard as they could, this time throwing them down afterward, onto either a padded surface or a metal bar. The measured forces went up by a factor of nearly 50. As the paper concludes: “The angular acceleration and velocity associated with shaking occurs well below the injury range, while the values for impacts span concussion, subdural, and diffuse axonal injury ranges.” That is, the data implied that shaking alone, at the velocities plausible at the hands of a normal adult, could not cause the symptoms commonly ascribed to shaking. These were impact injuries.
Duhaime’s team also reviewed all cases of SBS seen at the Children’s Hospital of Philadelphia between January, 1978, and March, 1985: In all 13 fatal cases, the infants had evidence of blunt impact to the head—although in more than half of the fatalities, that evidence was uncovered only at autopsy.
The authors concluded that
…the shaken baby syndrome, at least in its most severe acute form, is not usually caused by shaking alone. Although shaking may, in fact, be a part of the process, it is more likely that such infants suffer blunt impact. The most common scenario may be a child who is shaken, then thrown into or against a crib or other surface, striking the back of the head and thus undergoing a large, brief deceleration. This child then has both types of injury—impact with its resulting focal damage, and several acceleration-deceleration effects associated with impact causing shearing forces on the vessels and parenchyma.
By this time, the late 80s, SBS was showing up in the courtroom, as doctors who learned about Caffey’s research started reporting cases to the authorities. To the frustration of doctors in the field, then, the Duhaime research muddied the waters considerably. Defense attorneys could argue that no abuse occurred if the state couldn’t prove an impact, for example, when everyone knew that an impact with the bed would leave no marks.
The Duhaime study was quoted and argued at Stephanie’s trial, where it was essentially lost in the chaos. Although there was no evidence of bruising on Dinah Nelson’s scalp, the child did have an undatable skull fracture, which implied an impact at some point. Stephanie’s lawyer argued that the skull fracture had been inflicted earlier, and that Dinah’s evolving injury merely came to a climax while the infant was under Stephanie’s care. The prosecutor argued that Stephanie had abused Dinah in the past, and then “finally lost it” and brutally attacked the child one last time, minutes before the seizures started.
Because of Dinah’s skull fracture, I’d thought at first that the shaking/slamming debate had nothing to do with Stephanie’s case: clearly Dinah had suffered an impact, which is known to cause the symptoms. Did the lack of bruising on Dinah’s scalp mean that the fracture was old, though? Could you get a skull fracture from an impact with a pillow? And what about the old pools of blood in her brain?
I’d gone to the medical library looking for the research behind the key testimony that had convicted Stephanie: The doctors’ faith in immediate symptoms. What I’d found was a fundamental debate about the diagnosis itself.
(c) 2011 Sue Luttner
No further chapters posted yet.
[2] Yarnell, P. and Ommaya, A. “Experimental Cerebral Concussion in the Rhesus Monkey,” Bulletin of the New York Academy of Medicine, Vol. 45, No. 1, January 1969
[3] Ommaya, A.K., Faas, F., and Yarnell, P. “Whiplash Injury and Brain Damage: An Experimental Study” The Journal of the American Medical Association 1968; 204: 1968; 204: 75–79
[4] Gennarelli, T.A., Thibault, L.E., Adams, J.H., Graham, D.I., Thompson, C.J., and Marcincin, R.P., “Diffuse Axonal Injury and Traumatic Coma in the Primate,” Annals of Neurology 1982; 12: 564–574
[5] e.g., Ommaya, A., Mirsch, A., and Martinez, J. “The Role of Whiplash in Cerebral Concussion” Proceeding of the 10th Stapp Car Crash Conference, New York. Society of Automotive Engineers, 1966; pp. 197–203
[7] Duhaime, S.C., Gennarelli, T.A., Thibault, L.E., Bruce, D.A., Margulies, S.S., and Wiser, R., “The shaken baby syndrome: A Clinical, pathological, and biomechanical study,” Journal of Neurosurgery 1987; 66: 409–415.



Pingback: Innocent Family Petition Hits a Nerve | On SBS
Pingback: “Dissent Into Confusion:” The Supreme Court, Denialism, and Shaken Baby | On SBS
most brain injuries are caused by physical impact or accidents. *
Our own webpage
<a href=" http://www.foodsupplemendigest.com/vitamin-b12-overdose/ “
Pingback: Shaken: A Forensic Misadventure | Reporting on Health
Very good stuff Sue. you should talk to Ira Glass or one of the
RadioLab folks at NPR and do a show. at least.
Some thoughts in animal experimentation:
The summer after my freshman year in high school I had a job working
at SRI with an experimental psychologist. I built gadgets and ran
experiments on animals to investigate uremia
(http://en.wikipedia.org/wiki/Uremia) and electroanesthesia
(http://encyclopedia2.thefreedictionary.com/Electroanesthesia).
Though exciting for a 16-year-old wanna-be-scientist, the job, in
retrospect, seriously challenged my senses of morality and ethics.
At the time, I took for granted, that is was OK to partly remove a
monkey’s kidneys to simulate uremia so we could quantify their
degraded performance in cognitive and motor skills (push the red
button and get juice), and thought it OK to be using monkeys to
measure their reaction to electric shock induced pain while certain
portions of their brain was electrically stimulated in hopes of
finding how to induce an anesthetized state without drugs. I still
lay awake at night wondering if we were actually suppressing their
perception of pain, or simply impairing the animal’s ability to
vocalize when a pain threshold was reached.
along the way I read a paper or two on how researchers were putting
decerebrated cats on treadmills to investigate how gait limb
coordination was was regulated by spinal reflexes rather than higher
level motor coordination. This really gave me the creeps…
I got a few science fair awards out of the summer’s effort but it
definitely turned me off to animal experimentation. The hard
questions still remains: when is it OK (if ever) to torture animals
in order to improve the human condition, or gain knowledge.
The writing is so clear, so crisp, so good. I’m VERY impressed, young lady!
Nice work Sue – it reads like a NewYorker medical mystery article.
I am interested in seizures complicating whiplash injuries – have you any experience of such an association
My impression is that whiplash can cause neuronal damage that can trigger seizures, which quickly complicate the situation by interfering with breathing and more. I don’t have any literature citations to support this model. Maybe an intensivist could help you.
Fascinating, clear, beautifully written.
Kathryn
Sue, Great. First blog I’ve read written by a friend. Looking forward to reading more.
It was engaging and I learned zap much
Pictures and illustrations fab
Gail
WOW!!!
Run with it girl.
More later… need to assimilate.
Joe